Plantar Fasciitis Treatment: Persistent Heel Pain — and What Actually Works
Reviewed for Clinical Accuracy by Core Concepts Editorial Team
Related Articles
Plantar fasciitis is one of the most common causes of persistent heel pain. For many people, it comes and goes, flares unpredictably, and often lingers for months despite stretching, rest or changing shoes.
But the truth is this: Plantar fasciitis is rarely just a “foot problem”. It’s a load-management issue involving the foot, calf, ankle and your daily routines — and that’s why a single treatment approach doesn’t always create lasting results.
In this article, we dive into a case study of a client who was experiencing plantar fasciitis and how a collaborative physiotherapy + podiatry approach between Core Concepts Physio and Podiatry Quest helped a client break out of a persistent six-month pain cycle.
Meet Mr A: A Common Case of Stubborn Heel Pain
Mr A, 42, is a recreational runner who spends long hours standing at work.
He experienced:
- 6 months of right heel pain
- Sharp pain with the first steps in the morning
- Pain that worsened after long workdays
- Minimal improvement despite rest, stretching and shoe changes
He sought professional assessment and was diagnosed with plantar fascia–related heel pain.

Why His Pain Persisted: It Wasn’t Just the Foot
Many people think plantar fasciitis comes from “tight foot muscles” or “bad shoes”, but the condition is usually more complex. The foot and calf are meant to share load during walking and running.
When the calf can’t contribute effectively — due to limited ankle dorsiflexion, stiffness or reduced capacity — the plantar fascia absorbs more force than it can handle.
This leads to persistent, recurring pain.
Step 1: Physiotherapy Assessment
Mr A’s physiotherapist performed a full movement analysis and found:
- Calf stiffness and restricted ankle movement
- Reduced strength and load tolerance
- Poor single-leg control
- Running volume maintained despite pain
What this meant
His plantar fascia wasn’t the only issue — it was being overloaded from higher up the chain.
Physiotherapy Treatment: Improving Capacity

Physiotherapy focused on:
- Calf and ankle mobility
- Progressive strengthening for the calf, foot and hips
- Load management for standing and running
- Radial shockwave therapy (to support tissue healing)
- Education on flare-up management
After 4 weeks:
- Morning pain improved
- Running became more comfortable
- But heel pain still flared after long workdays
This indicated that capacity was improving, but daily load on the foot had not.
The Turning Point: Bringing in Podiatry
Instead of increasing exercises or intensifying treatment, our physiotherapist referred Mr A to our in-house podiatrist for a deeper look at foot mechanics and daily load patterns.
Podiatry Assessment: Understanding the Ground-Up Forces
The podiatrist identified:
- Prolonged foot pronation during walking
- High cumulative load from work footwear
- Poor shock absorption during long standing
- Increased plantar fascia strain during mid-stance
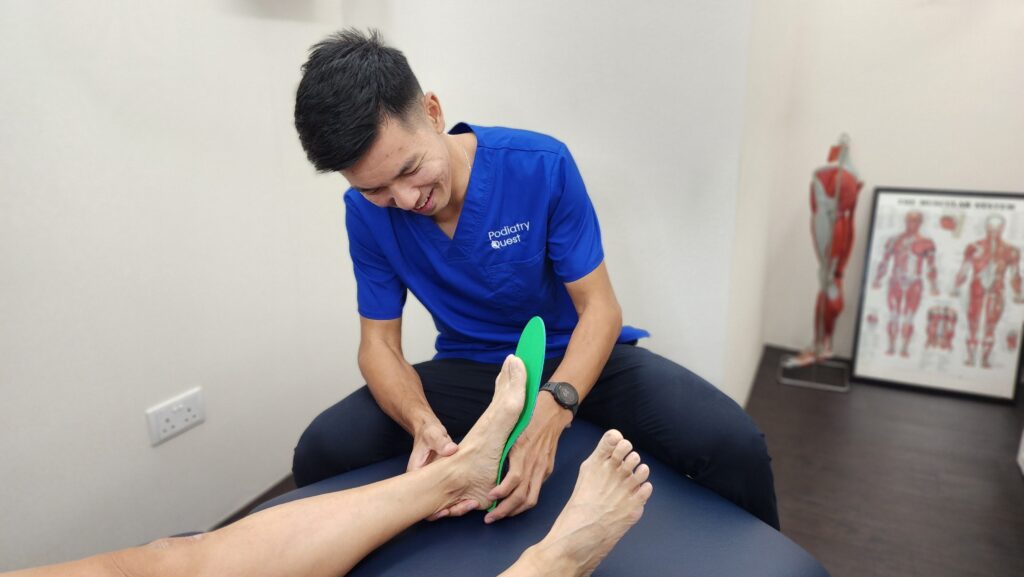
To address these, the podiatrist implemented:
- Customised foot orthoses
- Work and running footwear recommendations
- A gradual transition plan to prevent new overload
The effect:
Daily mechanical stress finally reduced, and Mr A’s symptoms began improving more consistently.
Why Collaboration Worked: Two Specialists, One Complete Solution
Physiotherapist’s role:
- Build strength
- Improve mobility
- Re-train load tolerance
- Correct movement patterns
Podiatrist’s role:
- Optimise foot mechanics
- Reduce strain entering the foot
- Improve footwear and ground contact
- Provide orthotic support
Together:
- Load was reduced and capacity was rebuilt
- No stones were left unturned
- Treatment addressed both the cause and the consequence
- Mr A received one plan, one direction — no mixed messages
Outcome: A Recovery That Finally Moved Forward
After 10 weeks of combined care:
- Pain-free first steps in the morning
- Able to stand long hours without heel pain
- Returned to his previous running volume
- Confident in managing load and symptoms
- No flare-ups at 3-month follow-up
This is the benefit of a fully optimised, collaborative treatment plan — especially for complex or stubborn plantar fasciitis.
What This Means for You
If you’ve been dealing with heel pain that keeps coming back, it may not be about doing more treatment — but doing the right combination of treatments.
A physiotherapist helps your body handle load.
A podiatrist helps your foot take load safely.
Together, they give you the best chance of lasting recovery.
At Core Concepts Physio, our multidisciplinary team includes both physiotherapists and podiatrists who work closely together to assess, diagnose, and treat complex conditions like plantar fasciitis. By combining clinical expertise across disciplines, we ensure that no stone is left unturned — and that every client receives a fully optimised, coordinated treatment plan tailored to their daily life, goals, and movement needs.
If you’re unsure where your heel pain is coming from or why it keeps returning, our team is here to guide you with clarity, confidence, and complete care. Book an appointment to speak to our team of physiotherapists!
Related Articles
- Plantar Fasciitis - Pain In The Heel! What is plantar fasciitis? Plantar fasciitis is a foot pain condition and a term given for the painful and inflamed…
- Rest Alone Isn’t Always the Answer for Plantar Fasciitis Why Rest Alone Isn’t the Solution for Plantar Fasciitis Many people with heel pain instinctively put their feet up, believing…
- Maybe it's not Plantar fasciitis but Heel Fat Pad Syndrome Do you have heel pain? And think it is Plantar Fasciitis? Maybe not, it might be another type of…
- Kneeling Pain: What Can I Do About It: Professional Insight Kneeling can be painful with existing knee pain. As a country often described as having a melting pot of cultures,…
- Top Effective Back Pain Treatment Is Not Bed Rest For Relief Low back pain is one of the most common reasons for consulting a physician. Despite little supporting scientific evidence,…
