
Urinary Incontinence – Why it happens and how to treat it
Reviewed for Clinical Accuracy by Core Concepts Editorial Team
Urinary incontinence (UI) is having a sudden, uncontrollable urge to pass urine that cannot be deferred, regardless of how full the bladder is. Experiences of UI can range from mild inconvenience to extremely disruptive and debilitating, both physically and emotionally. Many people find it to be a difficult problem to talk about. However, it may be far more common than you think – an estimated 50% of women and up to 11% of men experience UI worldwide. Of these, only a fraction seeks and receives treatment. Thankfully, there are many treatment options available, and they can be as easy as a few guided exercises at home to manage incontinence. Don’t let incontinence prevent you from going out and enjoying the things you love doing. Read on to find out the causes of urinary incontinence, treatment options, and helpful exercises to improve your symptoms.
Anatomy of the Pelvic Floor
The pelvic floor is a layer of muscles in the pelvis that connect the pubic bone to the tailbone. It helps to support the abdomen and control bladder and bowel movement. In particular, the internal and external urethral sphincter and levator ani act like a control valve around the urethra. To stop urine from passing through, these pelvic floor muscles must contract (squeeze) to close the urethra, which then stops the flow of urine.

Symptoms of Urinary Incontinence
Common symptoms of UI vary between people and can range from mild and temporary, to very disruptive and chronic. Some common symptoms include:
- Urine Leaking – uncontrolled passing of urine
- Urinary Frequency – needing to pass urine more frequently than usual, not from drinking more
- Urinary Urgency – having strong urges to pass urine, regardless of how full your bladder is
- Nocturia – disrupted sleep due to a need to pass urine
What Causes Urinary Incontinence?
Why does Urinary Incontinence happen? Common causes of urinary incontinence can be temporary or persistent.
Temporary causes of urinary incontinence can include:
- Urinary tract infections
- Ingesting diuretic foods or drinks, called bladder irritants (e.g. alcohol, caffeine, carbonated drinks and certain medications)
Persistent causes of UI are often a consequence of other underlying physical problems or changes, such as:
- Pregnancy: the growing baby causes more pressure on the bladder, and pregnancy hormones cause the pelvic floor muscles to loosen, making it harder to contract
- Childbirth: during childbirth stretching of the pelvic floor allows passage for the baby, making the pelvic floor muscles loose and weak, especially from a prolonged delivery or delivery of a large baby. This typically continues for up to 6 weeks after delivery before self-resolving, but can continue indefinitely if not treated
- Age-related changes: as you age the bladder becomes less stretchy and cannot store as much urine, forcing you to go to the toilet more frequently
- Being overweight: increased bodyweight, especially if it is around the midsection, places more pressure on the abdomen and bladder
- Constipation: excessive filling of the colon (where faecal material is collected before being passed) puts more pressure on the bladder
- Persistent heavy lifting: frequent increased intra-abdominal pressure while lifting puts more pressure on the bladder
- Menopause: oestrogen levels drop during menopause causing the pelvic floor muscles to loosen and become weaker
- Enlarged prostate (in men): as the prostate enlarges it can compress and block the urethra, stopping urine from passing through
It is common to have a weak pelvic floor in addition to the above conditions, which creates further difficulty in voluntarily controlling the flow of urine.
Treating Types of Urinary Incontinence
Urinary Incontinence is usually classified into 2 categories: Persistent UI and Temporary UI
1) Persistent UI
Treating the underlying causes of UI can be difficult, as things like childbirth and age-related changes have no specific treatment. However, pelvic floor control and strengthening exercises can help alleviate symptoms significantly and give you back control over your body.
Pelvic floor muscle training focuses on learning how to contract the pelvic floor muscles voluntarily to prevent urine flow. Examples include Kegels and pelvic floor squeezes. This is effective for improving symptoms of stress incontinence. Building strength and endurance in these muscles will help you maintain control over your bladder. A pelvic floor trained physiotherapist can assist with these exercises, as they are very specific and can be difficult to learn correctly by yourself.
In contrast, bladder training is a method of training your ability to hold urine for longer, by following a voiding schedule. This means you suppress the urge to relieve yourself till the scheduled time. This is effective for improving urge incontinence. In addition, ensuring good bowel habits to prevent constipation, ingesting fewer diuretic foods/drinks are also helpful behaviours.
2) Temporary UI
Treating temporary UI focuses on managing the aggravating food or drink which may have diuretic effects. These are called bladder irritants. Ingesting fewer bladder irritants will alleviate symptoms quickly, and will rarely need any further treatment.
Strengthening the Pelvic Floor
Here are some basic pelvic floor exercises to start with at home to strengthen the pelvic floor muscles. These exercises are beneficial for both men and women – For pregnant women, starting these exercises before pregnancy and continuing throughout will help to manage any UI post-partum. As you build the strength and endurance of these muscles, you can increase the repetitions and the number of times you do them a day.
1) Basic Pelvic Floor Squeeze
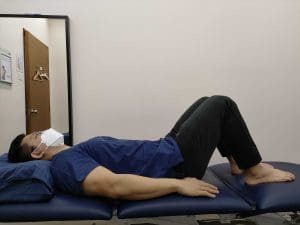
Stand, sit or lie with your legs slightly apart. Slowly tighten and pull up the pelvic floor muscles by squeezing like you need to go to the toilet. Make sure your abdominal wall and buttock muscles remain relaxed. Repeat 5-10 times, twice a day.
2) Squeeze and Hold

Start in the same position as the basic pelvic floor squeeze. Tighten and pull up the pelvic floor muscles, and hold for 5 seconds. If you can hold for longer, hold for up to 10 seconds. Repeat 5-10 times or until you are unable to maintain the squeeze. Do these exercises twice a day.
3) Fast Squeeze

In the same position, squeeze the pelvic floor muscles up as quickly as you can, and hold for 1 second. Fully relax, and repeat 5-10 times or until you are unable to maintain the squeeze. Do these exercises twice a day.
4) Squeeze with Leg Raises

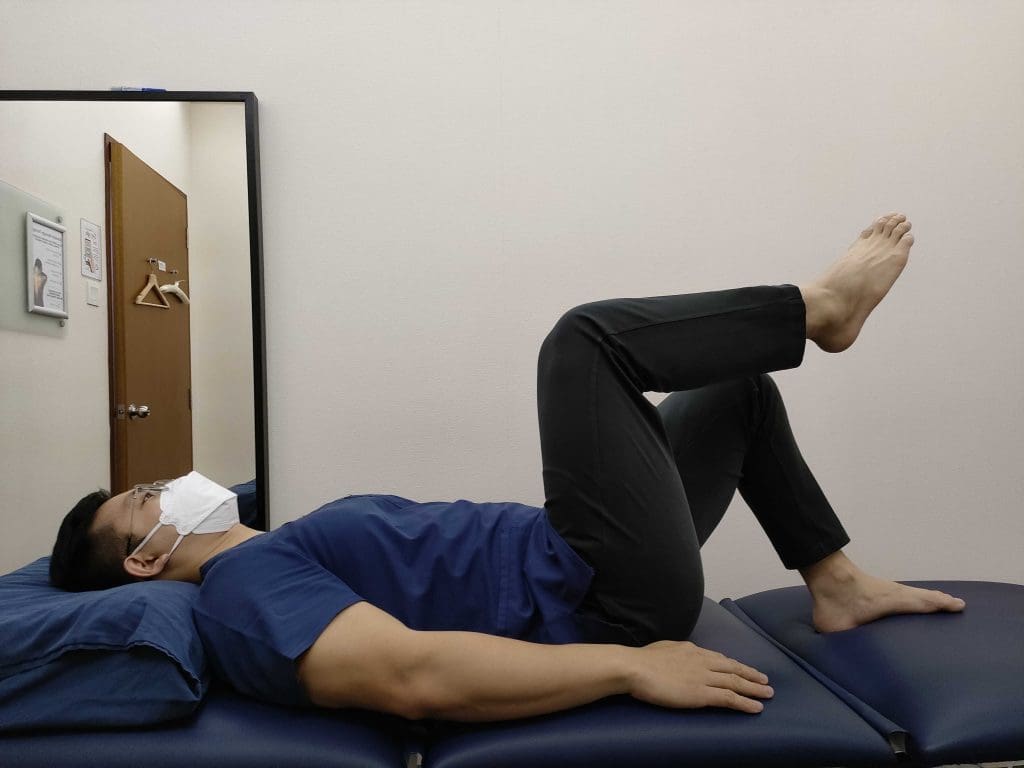
Lay on your back with knees up, with feet hip-width apart. Squeeze the pelvic floor muscles up and hold. While maintaining the squeeze, raise one foot off the floor – do not let the pelvic floor drop. Hold for 1 second, then place your foot back on the floor. Relax the pelvic floor completely. Repeat with the other leg. Repeat on both sides 5-10 times or until you are unable to maintain the squeeze. Do these exercises twice a day.
5) Squeeze and Stand



Start seated on a chair. Squeeze the pelvic floor muscles up and hold. While maintaining the squeeze, stand up from the chair, and sit back down. Relax the pelvic floor. Repeat 5-10 times, twice a day.
Seek Physiotherapy Help
Strengthening the pelvic floor can be puzzling at the start, as most people learned how to control them as a young child, and have never had to squeeze them consciously. If you have difficulty feeling the right muscles during these exercises, seek the help of a physiotherapist with pelvic floor muscle training. Our women’s health physiotherapy team will be able to help you with this as well.
While urinary incontinence can be troubling, it is not ‘normal’ and can be treated. There are simple management options available to you to help improve your quality of life. With some guidance from a trusted therapist and lifestyle changes, you can take back control of your body and get back to doing the things you love doing.
Related Articles
- Manage Incontinence - 7 Easy Tricks Remember when we mentioned having inconvenience during pregnancy? Urinary incontinence is one of the most common discomforts plaguing expectant mothers,…
- Empowering Women's Musculoskeletal Wellness:… As we celebrate International Women's Day, it's crucial to highlight the unique musculoskeletal health concerns that disproportionately affect women. Recent…
- The Importance Of Strong Pelvic Floor Muscles Explained One of the most significant problems faced during pregnancy is a weak pelvic floor. Strong pelvic floor muscles can help…
- Coping With Pregnancy Related Musculoskeletal… The majority of musculoskeletal problems that arise during pregnancy can be prevented and treated with physiotherapy intervention. Individualized physical therapy…
- Exercise Therapy: Coping With Pregnancy Related… Most of the musculoskeletal problems that arise during pregnancy can be prevented and treated by physiotherapy. Individualized physical therapy programs…
