
Basketball Injuries – 3 Common Injuries & How Physiotherapy Can Help
Reviewed for Clinical Accuracy by Core Concepts Editorial Team
Basketball has gained popularity around the globe since its creation 100+ years ago. With a standard hoop located 3+ metres (10 feet) off the ground, the sport requires a lot of jumping from the players during the game, and it is no surprise that fair bits of basketball-related injuries are affecting our lower limbs. This article will discuss the three common basketball conditions and how physiotherapy can help, as well as a case study of a basketball athlete client who came to us with a sports injury. Read on to find out how we were able to help!
3 Common Basketball Injuries
1. Ankle Sprain

Most basketball players have suffered ankle sprain before. It occurs when a player rolls his ankle, which results in the overstretching or tearing of one or more ligaments connecting the bones in the foot and the lower leg. The degree of damage (micro, partial or complete tear) on the ligaments determines the severity of the injury and the time required for recovery. Ankle sprains occur when a player lands awkwardly, on the floor or another player’s foot, usually during the landing after a jump shot, layup or dunk in the paint area. Players can also twist their ankles when changing directions at high speed during a crossover or stepback movement.

Inversion sprain is the most common mechanism of injury, where an ankle rolls inwards and tears the ligaments at the outer side of the ankle. The diagram below indicates the three common ligaments that are likely to be injured during an inversion sprain. Common signs and symptoms of ankle sprains include pain, swelling and bruising around the outer ankle, as well as pain when bearing weight on the injured ankle (e.g. walking, stairs, standing on one leg).
2. Tendinopathy – Patellar & Achilles Tendon
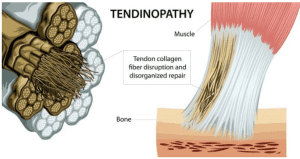
The second most common basketball injury is tendinopathy. A study followed the FC Barcelona Basketball Team for eight seasons and found out more than 40% of the players suffer from patellar tendinopathy or Achilles tendinopathy. Tendinopathy is typically an overuse condition, commonly known for its long-lasting and on-off pain around the tendons. Tendons are strong and elastic, with a role in absorbing and transmitting force between bones and muscles. Tendons are also sensitive to load. They are able to get stronger or weaker to match the load going through them. However, during scenarios such as returning from off-season, there is a sudden increase in activity level, hence the load increases rapidly and the tendons do not have enough time to get stronger to catch up with the new load. This results in inflammation in the tendons.
It is also common for people to develop tendinopathy symptoms in the midst of a season, as the tendons have been under heavier load, and usually without sufficient rest. If the inflammation is not addressed, tendons can be further damaged and its ability to absorb and transmit force can be affected. Therefore, people with tendinopathy may also have difficulty and pain when exerting the muscles around their affected tendon.
Most movements in basketball involve jumping, landing and quick turnings. As these are all generated by lower limb muscles, tendons at the knees and ankles are the most susceptible to tendinopathy. The patellar tendon can be found at the front of the knee, attaching the kneecap to the lower leg (tibia bone). It works closely with the muscles at the front of the thigh (quadriceps). The Achilles tendon connects the calf muscles (gastrocnemius and soleus) to the heel.
3. Patellofemoral Pain / Stress – Runner’s Knee
Runner’s knee is not exclusive to runners. It is also a common condition for basketball players who use their knees a lot due to the nature of the sport. This condition is characterised by a gradual build-up of dull aches around the area where the kneecap (patella) connects to the thigh bone (femur). Someone with patellofemoral stress may also have knee pain accompanying clicking or rubbing sounds when bending and straightening the knee, and/or a kneecap that is tender to touch.
There are three main causes for patellofemoral pain:
- Hip or thigh muscle tightness
- Muscle weakness
- Biomechanical factors (such as positioning of the kneecap, foot arch, and the way we walk or run)
These issues can also exist at the same time, affecting how well the kneecap and the knee joint move and work together.
How can physiotherapy help with these conditions?
1) Physiotherapy treatment for Ankle Sprain
- Pain and Swelling Management: The initial inflammatory phase of an ankle sprain can be quite achy and uncomfortable. Physiotherapy can help to reduce swelling and lower the pain level, ensuring adequate protection of the ankle for a proper recovery.
- Training – More Strength and Stability: It is common for basketball players to find their legs weaker and ankles less steady ankle sprains. With thorough assessments, physiotherapists can customise an exercise program that aids basketball players in returning to their beloved sport safely. Studies have also shown that stronger and steadier legs can minimise the recurrence of future ankle sprains.
2) Physiotherapy treatment for Patellar and Achilles Tendinopathy
- Pain Management: There are different phases of tendinopathy, and it is possible to have pain during any stage. Physiotherapy can help control the pain level and inflammation.
- Training – Stronger Tendons: The key to recovery for any tendinopathy is a gradual increase in the loading of tendons. Physiotherapists can provide exercises to strengthen the affected tendon(s) and muscles, and advise on what activities to participate in throughout different stages of tendinopathy (for example: when to resume training, or when to return to competition).
3) Physiotherapy treatment for Runner’s Knee
- Physiotherapists have multiple ways to assist with the pain level around the kneecap in both the short term, by decreasing the intensity of symptoms, and long term, by fixing the root cause(s). Treatments are tailored to every basketball player based on the assessment findings to tackle the reason(s) contributing to their painful knees. For instance, an individualised exercise program which includes recovery and strengthening exercises can aid with the strengthening of weaker muscles; physiotherapists can also loosen up tight muscles with deep tissue releases and teach self-stretches at home.
Case Study of a Client with a Basketball Injury
Miss K is a student who plays basketball for the university team. She came in after completing a competitive season and was experiencing some aches around the front of her left knee for 3-4 months. She experienced slight aches whenever she walked or stood for more than 3 minutes. Upon assessment with our physiotherapist, we found out that her left glute muscles were weaker and the muscles at the outer thigh were very tight. There was also some mild inflammation present around the kneecap. These affected how well the kneecap moved when she was playing basketball, especially when she was making sharp turns and fast jumps.
Physiotherapy Treatment Journey
The treatment journey for Miss K was broken down into 3 phases: managing the symptoms, building strength and basketball specific training for better performance and injury prevention due to the nature of her being a basketball athlete.
PHASE 1 – Symptoms Management (Duration: 2 weeks)
- The goal in this phase was to calm down the immediate symptoms as the knee was a bit irritated and slightly inflamed.
- Deep tissue release: We worked on the tight thigh and hip muscles on her left side of the body. This gave her an instant reduction in pain level during her normal day-to-day activities.
- Stretches and foam rolling: We taught Miss K how to loosen her tight muscles at home with stretches and a foam roller. She found these helpful in maintaining the effectiveness of the deep tissue releases and is able to cope with daily tasks much more comfortably.
- Ultrasound therapy: Miss K found ultrasound therapy helpful in reducing the pain and inflammation around the kneecap.
- Strengthening: We started building up strength for her since the first session. Strengthening the weaker glute muscles were the main focus. Our team adapted the strengthening exercises to be done lying down in this phase in order to let her inflamed left knee rest without irritating it.
PHASE 2 – Build Up Strength (Duration: 4 weeks)
- As her symptoms and discomfort in the knee improved, Miss K moved on to the next phase of the treatment journey where strengthening was the main focus.
- From our assessment, we knew that the main cause of her runner’s knee was due to weaker glute muscles on the left side. Hence, the main focus during this phase was to strengthen the weaker glute muscles in order to resolve the issues
- We progressed our exercises for Miss K with more loading through the knee, like squats and lunges to target her glute muscles.
PHASE 3 – Basketball Specific Training (Duration: 5 weeks)
- Once Miss K reached a certain level of strength, we shifted our focus towards getting her stronger in performing basketball-related tasks.
- Miss K was a point guard for the team, hence she needed to be able to do a lot of sharp and fast turns, as well as change in speed. Exercises like shuttle run and walk-run interval training are included in the individualised program to aid Miss K with her performance.
- Another aspect Miss K worked with us was her jumping during a layup. We helped her to be able to jump higher and further.
Miss K spent a total of 11 weeks with us in her rehab journey. Her symptoms were fully resolved and she was able to return to playing basketball pain-free. She reported that she felt stronger after her sessions and could perform better on the court. Hurray!
Seek Sports Physiotherapy for Basketball Injuries
The above case study was just an example of how physiotherapy can help with recovery and return to sports. The same condition can have different presentations, as well as different underlying reasons. If you are experiencing any pain or suspect that you may have a sports injury, do book an appointment with one of our physiotherapists to get your pain treated.
Related Articles
- Hiit Workouts: Check Your Form (Upper & Lower Body)… High-Intensity Interval Training (HIIT) is an increasingly popular and effective way to get lean. HIIT Programmes strip away the…
- Managing Sports Related Head Injuries And Concussion… In the earlier post, Concussion and Head Injuries in Contact Sports , we looked at the signs and symptoms of…
- Wimbledon Injuries: The 3 Most Notable Tennis… Welcome to the thrilling world of Wimbledon, where the best of the best battle it out on the hallowed grass…
- Bmt Injuries During National Service Explained Enlisting into National Service (NS) is a rite of passage in any Singaporean boy’s youth - some may find it…
- Rock Climbing: The Guide To Getting Started For… Rock Climbing for Beginners Rock Climbing for Beginners In this article, we will share tips on rock climbing for beginners.…
